Preparing The ICU Environment For a Child’s Visit
When prepared for the experience and surrounded by supportive caregivers who are able to create a safe environment for questions to be asked and grief to be experienced, children of all ages tend to benefit from having the option to say goodbye to a dying loved one.
When bringing a child onto an adult ICU, it’s likely that both the child and ICU staff might have some trepidation. It is extremely important to include hospital staff in the plan for bringing a child to bedside. Inclusion of bedside nurses, charge nurse, and social services allow for open communication as well as time to address any concerns staff might have about bringing a child onto the unit. It is the hope that this approach of working cohesively with the hospital team will ultimately make the outcome more comfortable for all parties involved.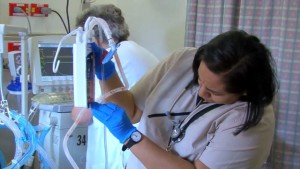
Step One: Present the situation for staff members who will be affected by the child’s visit.
This pertains not only to your bedside nurse, but others on the unit. The charge nurse is a key player in the visit, as they can help facilitate any special needs you might have. Present a clear picture as to who will be coming on the unit, the reason for the visit, and an estimation of how long the visit is planned for. It is helpful to let hospital staff know that you are working with the family’s wishes to facilitate an appropriate goodbye for the child.
Step Two: Once you have presented your plan for the visit it is important to acknowledge any concerns that hospital staff might have.
Listen carefully to concerns and address them. The culture and environment of each hospital will vary. Some adult ICUs do not allow children under 12 to participate in visitation. As a result, it is likely that some staff involved will be uncomfortable with the idea of a child coming to bedside. Take the time to acknowledge what they are saying; they might raise a point that will alter your plan.
Step Three: If concerns do arise, support those who are having difficulty with the plan.
Some concerns may be due to timing (change of shift, assessments, etc.) which we can work around. Other concerns may come from minimal experience of working with children who are grieving or simply the uncomfortable nature of seeing a child in emotional pain. Rely on institutional wisdom and what we know to be true about children and grief, and share what you know in a manner that is respectful.
Step Four: Take some time to really survey the scene.
 The ICU environment is an extremely foreign place for children. Be creative in finding ways to minimize the stress of the experience. Here are some things to consider while doing your survey…
The ICU environment is an extremely foreign place for children. Be creative in finding ways to minimize the stress of the experience. Here are some things to consider while doing your survey…
- Walk the path of the child (is there another more direct route?); if the child is small, get down low and take in that perspective (you might be surprised at how you feel).
- Is it possible to draw curtains or shut other patient’s doors?
- What is the bedside environment like; think of the senses (is it bright, is there a smell, what is the noise level) and are there ways to minimize these things?
- Work towards presenting the patient’s physical appearance to the child in the most appropriate manner.
- Where is the best place for the child to stand, sit, etc.?
Once your survey is complete you may have requests or require assistance from hospital staff. Never assume that it is okay to execute your requests without consulting with hospital staff; for example, drawing curtains or shutting doors. Again, go back to step one. Hopefully the groundwork you have laid with the hospital staff from earlier will make the facilitation of your needs a much smoother process.
Cherry Wise began working in the OPO field in 1997 when she had a private practice as a psychologist and was a professor at the Wright Institute of Professional Psychology in Berkeley. Previously she was director of a non-profit organization that provided services to children and their families in times of bereavement or impending loss.

